10 Risk Factors of High Body Mass Index (BMI)
The purpose of this report is to highlight and explain the health risks associated with a high Body Mass Index (BMI). BMI is a widely used indicator to assess an individual’s body fat based on height and weight.
While it is not a perfect measurement of overall health, it serves as a useful guideline in identifying individuals who may be at increased risk for various health conditions. As BMI increases, so does the likelihood of developing a wide range of serious medical issues, many of which can severely affect quality of life and even shorten lifespan.
This report outlines ten major health risks linked to high BMI, emphasizing the importance of maintaining a healthy weight for overall well-being.
1. Increased Risk of Infection Post-Surgery
Surgical procedures inherently carry a risk of infection; however, individuals with a high BMI are at significantly greater risk. Excess fat tissue tends to have a reduced blood supply, which slows healing and impairs the body’s ability to fight off infection. As a result, wounds may take longer to close, increasing the chance of bacterial growth and complications.
Additionally, surgeries on obese patients are often more complex due to the presence of excessive fat tissue, which can make the procedure technically challenging and time-consuming. These extended durations under anesthesia and in the operating room can further elevate the infection risk. Surgeons often must take special precautions when operating on obese patients.
Patients with high BMI who undergo surgery may also be more prone to developing chronic wound infections or surgical site infections (SSIs), which can lead to prolonged hospital stays, the need for additional surgeries, or even life-threatening conditions like sepsis. Preventive care, weight management, and early intervention are crucial to reduce these risks.
2. Increased Risk of Arthritis in Knees and Hips
The joints in the body, particularly those in the knees and hips, are built to withstand a certain amount of stress. Carrying excess body weight increases the pressure on these load-bearing joints, accelerating the natural wear and tear that comes with age and physical activity. Over time, this can lead to osteoarthritis, a degenerative joint disease characterized by stiffness, pain, and reduced mobility.
Research has shown that for every extra pound of body weight, an additional four pounds of pressure is exerted on the knees. This exponential increase in joint stress explains why obesity is so strongly linked to joint problems. The cartilage that cushions joints wears away faster, causing bones to rub against each other, resulting in chronic pain and inflammation.
People with obesity often find themselves in a difficult cycle—joint pain limits their ability to exercise, and lack of physical activity further contributes to weight gain. Early weight management and low-impact physical activity like swimming or cycling can help reduce joint strain and prevent the onset of arthritis.
3. Increased Risk of Sleep Apnea
Obstructive sleep apnea is a serious condition where the airway becomes repeatedly blocked during sleep, leading to interrupted breathing and poor-quality rest. Individuals with a high BMI are at significantly higher risk for sleep apnea because excess fat around the neck and upper airway can cause narrowing or complete obstruction of the airways during sleep.
This condition doesn’t just affect sleep quality—it has a cascade of negative effects on overall health. Poor sleep can lead to daytime fatigue, difficulty concentrating, mood disorders, and increased risk of accidents. Over time, untreated sleep apnea also contributes to high blood pressure, heart disease, and type 2 diabetes.
Fortunately, sleep apnea is treatable. Weight loss is one of the most effective interventions, as even modest reductions in weight can significantly reduce the severity of the condition. In addition to weight management, treatments may include the use of CPAP (Continuous Positive Airway Pressure) machines and lifestyle changes.
4. Increased Risk of Diabetes
One of the most well-known and concerning risks of high BMI is the development of type 2 diabetes. Excess body fat, particularly around the abdomen, is associated with insulin resistance—a condition where the body’s cells no longer respond effectively to insulin. When insulin can’t properly regulate blood sugar, glucose builds up in the bloodstream, leading to diabetes.
Individuals with obesity are not only more likely to develop diabetes, but they also tend to experience more complications. High blood sugar over time can damage blood vessels, nerves, kidneys, eyes, and other organs. It also increases the risk for cardiovascular disease and infections.
The encouraging news is that type 2 diabetes is often preventable and even reversible with lifestyle changes. Losing weight, eating a balanced diet, and increasing physical activity can dramatically improve blood sugar control and reduce the need for medications.
5. Increased Risk of Blood Clots
A high BMI often contributes to a sedentary lifestyle and poor circulation, which increases the risk of blood clots, especially in the legs—a condition known as deep vein thrombosis (DVT). These clots can travel to the lungs and cause a pulmonary embolism, a potentially life-threatening complication.
Obesity also leads to inflammation and changes in the blood’s ability to clot properly. Fat cells release substances that make blood thicker and more prone to clotting. This risk is further compounded by long periods of immobility, such as during long flights or hospital stays.
Preventive strategies include regular movement, compression stockings, hydration, and, for those at high risk, anticoagulant medications. Maintaining a healthy BMI and staying physically active are among the most effective ways to prevent clot formation.
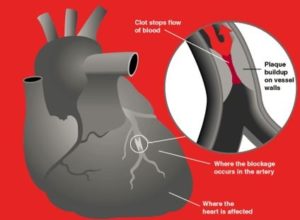
6. Increased Risk of Stroke
Stroke occurs when blood flow to part of the brain is interrupted, leading to brain cell death. People with high BMI are at increased risk of stroke largely due to associated conditions like high blood pressure, high cholesterol, and type 2 diabetes. These conditions damage blood vessels and make blockages more likely.
Obesity also contributes to inflammation and hardening of the arteries (atherosclerosis), further increasing stroke risk. Central obesity, or fat around the abdomen, has been particularly linked to higher stroke rates, even in individuals who are otherwise healthy.
Reducing BMI can significantly lower stroke risk. Lifestyle changes that address weight, diet, and activity level can help control the underlying conditions that contribute to stroke, offering both immediate and long-term protective benefits.
7. Increased Risk of Gallbladder and Fatty Liver Disease
Obesity is a major risk factor for gallstones—hard deposits that form in the gallbladder and can cause severe pain, nausea, and infection. Rapid weight gain or loss can also trigger gallstone formation. Gallbladder disease often leads to surgery and digestive issues.
In addition, excess fat can accumulate in the liver, leading to non-alcoholic fatty liver disease (NAFLD). This condition reduces the liver’s ability to function properly, affecting metabolism, detoxification, and nutrient storage. If left untreated, NAFLD can progress to more serious liver conditions such as fibrosis, cirrhosis, or even liver failure.
Maintaining a healthy weight through balanced nutrition and regular exercise is key to preventing these issues. In many cases, reducing BMI can reverse fatty liver changes and improve gallbladder function, minimizing long-term health risks.
8. Increased Risk of Infertility
High BMI can disrupt the delicate balance of hormones involved in reproductive function. In women, this often leads to irregular menstrual cycles and ovulation issues, making it harder to conceive. Obesity is also associated with polycystic ovary syndrome (PCOS), a common cause of infertility.
In men, obesity can lead to decreased testosterone levels and lower sperm quality. Excess body fat produces estrogen, which can disrupt hormonal balance and reproductive function in both sexes. This hormonal imbalance can delay or prevent conception.
Fortunately, even modest weight loss can restore hormonal balance and improve fertility outcomes. Healthcare providers often recommend weight management as the first step in fertility treatment for individuals with high BMI.
9. Increased Risk of Kidney Stones
Kidney stones are hard deposits made of minerals and salts that form inside the kidneys and can cause intense pain when passing through the urinary tract. Studies show that people with high BMI are more likely to develop kidney stones due to metabolic changes that alter the composition of urine.
Obesity increases the excretion of substances like calcium, oxalate, and uric acid in the urine, all of which contribute to stone formation. Additionally, diets high in salt, sugar, and animal protein—often associated with obesity—can raise stone risk further.
To reduce the risk of kidney stones, individuals with high BMI should aim to stay hydrated, reduce intake of salt and sugary foods, and manage their weight through dietary changes and increased physical activity.
10. Increased Risk of Gout
Gout is a painful form of arthritis caused by the buildup of uric acid crystals in the joints. Individuals with high BMI are more likely to experience elevated levels of uric acid in the blood, a condition known as hyperuricemia, which is the primary trigger for gout attacks.
Obesity interferes with the kidneys’ ability to eliminate uric acid, causing it to accumulate in the bloodstream. This leads to the formation of sharp crystals, particularly in the toes, feet, and ankles, resulting in swelling, redness, and intense pain.
Lifestyle changes such as losing weight, limiting intake of purine-rich foods (like red meat and seafood), and avoiding sugary drinks can help lower uric acid levels and prevent gout flare-ups.
A high Body Mass Index is far more than a number on a scale—it is a warning sign of potential health complications that can affect nearly every system in the body. From chronic conditions like diabetes and arthritis to acute emergencies like stroke and pulmonary embolism, the risks are both serious and wide-ranging. The good news is that many of these risks can be reduced, and even reversed, through weight management and lifestyle changes.
Recognizing the risks is the first step toward prevention and improved health outcomes. With the right support, resources, and mindset, individuals can take control of their health and reduce the impact of high BMI on their lives.