Prevent Heart Disease by Learning About Your Heart
Your heart is one of the most important organs in your body. Learn about its anatomy and functions so you know how to prevent heart disease.
Prevent Heart Disease by Learning About Your Heart
Your heart is directly involved in supplying all of your organs with the oxygen they need to function properly. Without it, your body would completely shut down. This is why it’s so important to take good care of your heart.
If you develop heart disease, your heart is no longer able to perform its primary function with the same efficiency.
Learning more about the anatomy and functions of your heart can help you understand not only the role it plays in your overall well-being but also how you can take better care of it to avoid heart disease.
Functions of the Heart
Each day, your heart pumps about 2,000 gallons of blood if it’s functioning regularly. Your heart is a key component in keeping your blood cells oxygenated and delivering this oxygenated blood throughout your body.
Oxygenating Blood
Your cells could not perform their regular functions without oxygen, and oxygen fuels cellular respiration, which is where your cells use oxygen to break down nutrients into energy and waste. The waste gets discarded, and the energy is used as fuel for your body. Since oxygen is such an integral part of your cells’ regular functions, your body has to ensure a constant supply is reaching your cells at all times, which is accomplished by oxygenating your blood. The heart doesn’t supply this oxygen itself, but it does facilitate oxygenation by pumping deoxygenated blood into the lungs.
Circulating Blood
Once blood has been oxygenated, it moves from the lungs back into the heart. It then has to reach the rest of your body. Your heart pumps this blood through your arteries, which carry it to organs and tissues throughout your body. Contractions, known as heartbeats, push blood through your circulatory system. Once the oxygen is used up, blood returns to the heart to be oxygenated once again.
Anatomy of the Heart
Your heart is a complex organ made up of a series of chambers, valves, and tissues. Each part of the organ is involved in circulating your blood throughout your body, and damage to any of them can jeopardize your health.
Chambers
Your heart consists of four chambers. You have left and right atria located in the upper area of the heart and left and right ventricles in the lower area. The left and right sides are separated by a muscle wall known as the septum.
Blood enters your heart through the atria from your veins. It passes from the atria into the ventricles, which then pump the blood out of the heart.
The atria are thinner than the ventricles, as not as much force is needed to transfer blood between the chambers of the heart. More force is needed to pump blood out through the arteries.
The right atrium receives deoxygenated blood and passes it through to your pulmonary system via the right ventricle. Your left atrium receives oxygenated blood from your lungs, which is then pumped out from your left ventricle to the rest of your body.
Valves
Heart valves control the flow of blood through the heart, ensuring everything stays moving in the right direction.
Atrioventricular valves, also known as cuspid valves, are located between the atria and ventricles. They close as the ventricles contract, preventing blood from flowing backward into the atria once it has passed into the ventricles.
Your heart also contains semilunar valves, which are located near the bases of the ventricles. These valves close and the ventricles relax, and these actions keep blood from flowing back into the ventricles after it’s been pumped out into your circulatory system.
Blood Vessels
Your heart is connected to many different blood vessels that carry blood to and from different cells and organs. These include both veins and arteries. While your veins bring deoxygenated blood back to your heart, your arteries pump oxygenated blood out of your heart and through your body.
Your largest artery, the aorta, brings blood to many different areas through smaller branches. You also have the superior and inferior vena cava, which bring deoxygenated blood back to the heart from your upper and lower body, respectively.
Your pulmonary artery and veins carry blood between your heart and lungs.
Your heart needs oxygenated blood to function too. This is supplied by the coronary arteries.
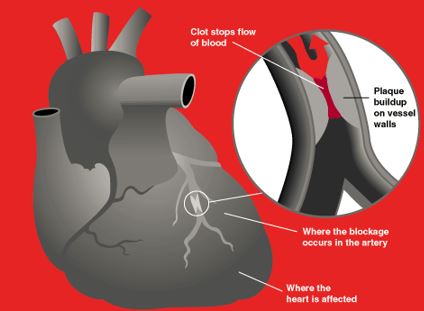
How Heart Disease Interferes With These Functions
Heart disease interferes with the regular function of your heart by restricting blood flow. Plaque builds up in your arteries, causing them to narrow, which in turn, limits how much blood can pass through them.
Without proper oxygenation in your heart and other parts of your body, your cells won’t have the energy they need to function properly. This can lead to major complications, like a heart attack.
Improving Your Health Through Heart Disease Treatment
Thankfully, there are many ways to keep your heart healthy and prevent heart disease. Common heart disease treatments include following a heart-healthy diet, quitting smoking, and getting more exercise.
Final Thoughts
Properly caring for your heart allows it to function efficiently. The more heart-healthy choices you make, the easier it is for your heart to continue to oxygenate and circulate blood like it’s designed to do.
5 Major Causes of Heart Disease You Should Avoid
Heart disease has many contributing factors that can increase your risk, but these five major causes are most commonly linked with developing heart disease.
So many of the choices you make every day can impact your heart health.
Choosing to exercise and eat right every day is a decision that helps keep your heart in good working order, while opting to lay on the couch and eat junk food doesn’t do you any favors. Despite how straightforward this might sound, you might not realize just how much of an effect these decisions have on the health of your heart.
This is especially important for habits that negatively impact key risk areas like your cholesterol and blood pressure. These factors, among others, are some of the leading contributors to heart disease.
Keep a careful eye on the five major causes of heart disease so you can understand and reduce your risk of developing this condition and maintain your overall health.
Major Causes of Heart Disease
In most cases, heart disease is the result of genetics or poor health caused by smoking, high cholesterol, high blood pressure, and uncontrolled diabetes.
Smoking
The most common danger associated with smoking is lung disease, but it can affect other parts of your body too. Smoking can make you two to four times more likely to develop heart disease than a non-smoker, especially if you smoke a pack or more every day. Smoking can damage your blood vessels, restricting blood flow. It also raises your blood pressure and heart rate, forcing the heart to work harder to supply your organs with oxygenated blood.
High Blood Pressure
High blood pressure has been connected to a number of different complications, but heart disease is among the most prevalent. When your blood pressure is high, your arteries become damaged over time. Plaque builds up and narrows the arteries, and the heart pumps faster and harder to maintain blood flow. The extra effort enlarges the left ventricle, weakening your heart and often resulting in congestive heart failure.
Diabetes
Diabetes can significantly increase your risk of heart disease, as high blood sugar damages your blood vessels.
When you have diabetes, your body’s ability to produce nitric oxide is reduced. Nitric oxide functions as a vasodilator, which means it widens your blood vessels. Without it, your blood vessels narrow, restricting blood flow.
Additionally, high blood pressure frequently occurs alongside diabetes, which increases your risk even further. This can manifest in peripheral artery disease (PAD), which limits blood flow to the legs.
High Cholesterol
Some cholesterol is necessary for your body to function regularly, but too much can lead to heart disease. This is because high cholesterol increases the amount of plaque in your blood vessels. Too much plaque narrows the vessels and inhibits blood flow.
If too much plaque builds up, these deposits can form a blockage that causes a stroke or heart attack.
Family History
Genetics can play a role in determining your likelihood of developing heart disease too. You’re more likely to have issues with blood flow and heart disease if a family member has it, especially if one of your parents or siblings has a heart attack before they turn 50.
Of course, this doesn’t mean you are fated to develop heart disease no matter what. With careful management of your health, including regular checkups with your doctor and a commitment to making heart-healthy choices, you can reduce your risk.
Reducing Your Risk Level
In many cases, reducing your risk of developing heart disease means adjusting your behaviors and taking your overall wellness seriously. You can keep your blood vessels in good working condition by making small changes to your daily habits and speaking to a medical professional.
Avoiding Harmful Behaviors
For causes of heart disease like smoking, the best thing you can do for your body is quitting. Smoking can damage many different organs and tissues throughout your body, not just your heart, so you should strive to stop as soon as possible.
If you’re having trouble quitting, at least reduce the number of cigarettes you smoke in a day. Heavy smokers have a much higher risk of damaging their hearts, and becoming a light smoker can reduce your dependency and make quitting easier.
Treat the Root Causes
Many forms of heart disease treatment involve focusing on the root causes of damage to the heart and blood vessels.
This means making healthier choices on a regular basis.
For example, you can lower your cholesterol and blood pressure by adjusting your diet. Cutting out saturated and trans fats, keeping your sugar consumption under control, and decreasing your salt content in your diet are all excellent healthy behaviors.
Getting just 30 minutes of exercise each day helps treat these conditions as well. Include some cardio to improve your heart health.
Speak With a Doctor About Heart Disease Treatment
If you have a family history of heart attacks and strokes, talk to your doctor about monitoring your risk levels at your yearly medical appointments. Keeping track of changes in your blood pressure and cholesterol can help you get on top of any issues through lifestyle changes or medication treatment.
Final Thoughts
The causes of heart disease come in many different forms, and all of them are dangerous. If you are affected by any of these causes, you should be more vigilant about taking good care of your heart to keep yourself healthy and strong.
Modern Advances in the Treatment of Heart Disease
Modern Advances in the Treatment of Heart Disease
Heart disease treatments have come a long way over time, with scientists continually developing new methods of addressing heart disease symptoms and root causes.
Modern medical knowledge is constantly improving as scientists work to develop a better understanding of the intricate systems at work in our bodies. This includes how our hearts function and the effect heart disease has on our bodies.
As we learn more about the processes that ensure our hearts function properly, heart disease treatments improve. This means the quality of life and longevity for people who have heart disease improves as well.
A Better Understanding of Heart Disease
Many of the treatments used to counteract the effects of heart disease today would be impossible without our modern understanding of the heart.
For example, because we know that restricted blood flow is a result of narrowed or blocked arteries, we can use devices like cardiac stents to reopen these arteries. Pacemakers and defibrillators are the results of the improved understanding of electrical physiology of the heart.
New advancements are being made every day, led by institutions like the American Heart Association with thousands of studies all over the world.
Developments in Heart Disease Treatment Methods
As knowledge and understanding of heart disease continue to improve, so do the methods used to diagnose and treat the condition.
Early heart disease treatments were limited to mainly lifestyle changes and some medications. While these methods can be effective for many people and are still used today, they are less effective in severe cases of heart disease.
Now that scientists and researchers better understand the mechanics of heart disease and its complications, they have helped create new and improved heart disease treatment methods. Many of these methods involve the surgical implantation of devices near the heart that help to control its rhythm and support its regular function.
Cardiac Stents
Heart disease leads to plaque buildup in your arteries, which narrows them and prevents regular blood flow. To treat this, cardiologists can insert a cardiac stent inside a blocked artery in a minimally invasive procedure known as coronary stenting.
A cardiac stent is an expandable metal mesh coil that’s small enough to travel through an artery. The stent is inserted with a balloon that expands when it reaches the blocked or narrowed section. The stent expands to keep the artery stretched wide enough for regular blood flow, and the stent stays in place, keeping the artery open after the balloon is deflated.
Coronary angiograms are emergently performed at the time an acute heart attack occurs, and the cardiologist will likely place a cardiac stent even if you have only one or two blocked arteries. Sometimes, there are several coronary arteries that are blocked, which requires more invasive procedures to treat.
Pacemakers
Normally, your heart serves as its own pacemaker. The sinoatrial (SA) node controls the rhythm of your heartbeats with regular electrical pulses that instruct the heart to contract and relax.
Heart disease can interfere with this regular rhythm. You may experience heart rhythm disturbances known as arrhythmias or palpitations, which can speed up or slow down your heartbeats. Any disturbance can interfere with how efficient your heart is at maintaining good circulation throughout your body.
To correct this issue, your doctor may suggest you undergo surgery to have a pacemaker implanted. The pacemaker monitors the rhythm of your heartbeats for irregularities and creates its own electrical impulses that restore the regular rhythm of your heart.
Defibrillators
If you are at a high risk of experiencing cardiac arrest, you may need an implantable cardioverter defibrillator (ICD). During cardiac arrest, your heart stops pumping effectively, and it may stop altogether, suddenly cutting off blood flow completely. This is life-threatening if you cannot get emergency medical treatment right away.
An ICD monitors for irregularities in the heart’s rhythm, specifically in the ventricles. If you experience ventricular arrhythmia, the ICD will deliver small electric signals to restore the heart’s regular rhythm. If this arrhythmia persists, it will deliver a large shock similar to a regular defibrillator to jumpstart the heart’s regular rhythm once again.
Note that sometimes these shocks can be painful, but they can also save your life. Some newer ICDs also serve the same function as pacemakers, stimulating heartbeats when your heart rate becomes too slow.
Final Thoughts
While heart disease treatments have come a long way, they are by no means perfect. You may have complications from the surgery needed to implant a pacemaker or defibrillator, and you may have to avoid things that could interfere with these devices, such as metal detectors and MRI machines.
Despite this, these are still significant improvements in how we handle heart disease. The more we continue to learn about the condition, the better equipped we will be to treat it safely and effectively.
3 Major Complications Caused by Heart Disease
Heart disease can cause serious and lasting damage to your body. Learn about the three most common major complications that come from heart disease.
If you have heart disease, your heart is less efficient at pumping blood. The blood vessels throughout your body, which facilitate blood flow to various organs, may be damaged as well.
These conditions can have significant harmful effects on your heart as well as your other organs. The harder your heart has to work to maintain your body’s circulation, the more likely it is that you will experience a major complication from heart disease.
Heart Disease’s Major Complications
Heart disease can cause health issues that affect your heart, such as heart attacks and congestive heart failure. It can also cause renal failure.
Heart Attack
Heart disease can limit not only the blood flow throughout your body but also the supply of blood to your heart. The proper supply of oxygenated blood can be restricted due to plaque buildup in your coronary arteries, in a condition known as coronary artery disease.
This is the primary cause of heart attacks.
During a heart attack, the cells in your heart don’t receive enough oxygen, and without oxygen, the cells start to die.
Common symptoms of a heart attack include chest pain, shortness of breath, and pain in other areas of your upper body like your arms, jaw, and neck. These symptoms can vary between men and women, with women being more likely to experience jaw or back pain and shortness of breath in addition to or sometimes instead of chest pain.
If you experience chest pain or otherwise believe you might be having a heart attack, seek medical treatment immediately. It is better to be overly cautious than to ignore the symptoms when you are really having a heart attack.
Congestive Heart Failure
Congestive heart failure is also caused by the narrowing of the arteries that supply blood to your heart due to plaque buildup. It is named after the ‘congestion’ that occurs in body tissue when blood is unable to circulate properly. This often causes swelling in the legs and ankles.
Heart failure can also be systolic or diastolic.
Diastolic heart failure means your heart isn’t properly relaxing between beats, while systolic means it isn’t properly contracting.
Renal Failure
Chronic kidney disease affects about 14 percent of the population, with one of its most common causes being high blood pressure.
Long-term high blood pressure, or hypertension, damages the arteries that supply blood to your kidneys, leaving them unable to filter waste in your blood properly. Damage to your blood vessels from heart disease can make this worse and speed up the progression of kidney disease to renal failure.
In the state of renal failure, your kidneys are no longer able to filter blood on their own. Renal failure is irreversible, and if left untreated, can be life-threatening. If you cannot get a kidney transplant, you will have to go on dialysis for the remainder of your life.
Avoiding These Complications
The most effective way to reduce your risk of having a heart attack, congestive heart failure, and renal failure is to target the factors that put you most at risk of developing heart disease in the first place.
Heart Disease Treatment
Many heart disease treatment methods involve lifestyle changes, which can be used to improve your health, whether you already have the warning signs of heart disease or not. Improve the strength of your heart by practicing routine exercise and avoiding eating too much fat, sugar, and sodium. Making these small changes can have a significant impact on your health.
If you already have heart disease, speak to your doctor about your concerns about developing heart complications. They will advise you on potential lifestyle changes, or they may recommend medication treatment.
Kidney Disease Treatment
Since heart disease can interfere with blood flow to the kidneys, take steps to improve the health of your kidneys too.
Kidney-friendly diets are low in protein, and they avoid minerals that are harder for your kidneys to process, such as phosphorus and potassium. Nutrition plans like the renal diet emphasize whole grains, fruits, and vegetables as part of a balanced meal.
It’s just as important to avoid excess sodium and fat in your diet for your kidneys’ sake as it is for your heart’s sake, and exercise can help here as well. Heart-healthy and kidney-friendly lifestyles are compatible with each other, and it’s a good idea to follow both if you want to prevent heart and kidney disease.
Final Thoughts
The complications of heart disease can be life-threatening, and you must make every effort to try to prevent their occurrence. Always take heart disease seriously and do your part in managing the condition before it results in a heart attack, congestive heart failure, or renal failure.
Understanding Heart Disease’s Connection to Arrhythmias
Heart rhythm disturbances, or arrhythmias, aren’t always a cause for concern. But they can be troubling when they occur as a result of heart disease.
Normally, your heart beats at a steady pace between about 60 to 100 beats per minute (bpm). However, in some cases, your heart may beat faster, slower, or in an irregular rhythm.
This is known as heart arrhythmia.
In many cases, a heart arrhythmia is only temporary and goes away on its own. That said, you should never let a heart arrhythmia continue without seeing a doctor. When it occurs alongside heart disease, it can be dangerous and, in some cases, life-threatening.
What Is Heart Arrhythmia?
Your heart has a natural pacemaker known as the sinoatrial (SA) node. This node controls the rhythm of your heartbeats with electrical impulses.
Under normal conditions, the electrical impulses ensure your heartbeats are steady and strong at a measured pace. If you are experiencing an arrhythmia, these impulses may be too fast, too slow, or off-rhythm, which in turn affects the pace of your heartbeats.
Rapid Abnormal Rhythms
Resting heart rates over 100 bpm are considered rapid abnormal rhythms. This is known as tachycardia, and it can feel like a fluttering sensation in your chest that leaves you feeling faint, dizzy, or out of breath.
Note that to be considered tachycardia, your heart rate must be measured when you’re at rest. Having a faster heart rate during and immediately after exercise is perfectly normal. But if you are sitting on the couch without exerting yourself, a fast heart rate is abnormal, and it could be a cause for concern.
You may experience tachycardia in the atria of your heart or in the ventricles. It often weakens the pumping of your heart, which can reduce blood flow.
Slow Abnormal Rhythms
If your heart rate falls below the lower limit of a regular resting rate, 60 bpm, this is considered a slow abnormal rhythm.
It is also known as bradycardia.
Like tachycardia, having a slightly slower heart rate isn’t always a bad thing. In fact, if you get a lot of exercise and you’re very physically fit, you may have a slower average heart rate. Your bpm may also fall below this level when you are sleeping or if you are taking medication for high blood pressure.
That said, if none of these conditions apply to you, persistently slow heartbeats could indicate your body isn’t getting an adequate supply of oxygenated blood. Bradycardia can also coincide with skipped heartbeats in some cases.
Irregular Rhythms
You may still have a heart arrhythmia if you don’t experience persistent slow or fast heartbeats, but instead, you feel like your heart occasionally skips a beat or beats prematurely.
This is considered an irregular rhythm.
While these heart palpitations can be uncomfortable, they’re not usually serious if they occur without any other symptoms. If you have chest pain, struggle to breathe, feel dizzy or lightheaded, or you faint alongside heart palpitations, you should seek medical treatment.
One of the most common causes of irregular heartbeats is atrial fibrillation (AFib).
The symptoms of AFib are shortness of breath, palpitations, or even persistent pain similar to a heart attack. Your heart rate may also be very fast, or it can be a normal rate.
AFib can increase your risk of having a stroke or heart failure.
Heart Arrhythmia and Heart Disease
Heart arrhythmias can occur as an isolated event, but they’re usually more serious if they occur alongside heart disease. Conditions like diabetes and high blood pressure can lead to more severe forms of heart rhythm disturbances, as can other heart disease risk factors such as smoking and high cholesterol.
Arrhythmia and Heart Disease Treatment
Sometimes heart arrhythmias are caused by underlying initial damage to the heart, such as can be seen with early heart disease. This means that it’s very important to begin utilizing common heart disease treatment strategies like eating healthier, getting more rest, quitting smoking, and exercising more frequently as soon as possible.
Speak to your doctor about any irregularities with your heart right away. They will help you identify the problem and help you find the best treatment regimen for the problem. This may involve prescription medications and consulting a cardiologist for their expertise in treating the problem.
Certain anti-arrhythmic medications and blood thinners can help bring rapid heart rates under control. In some cases, you may need an implantable device like a pacemaker or defibrillator to reduce your risk of cardiac arrest. These devices regulate your heart rhythms by creating their own electrical impulses.
If you have extensive coronary artery blockages in addition to any arrhythmia, you may need coronary bypass surgery to restore proper blood flow to your heart and help treat the arrhythmia.
Final Thoughts
Heart palpitations and other irregularities can be benign or sometimes severe problems. It’s best to always seek advice from a doctor who can identify the underlying cause of these conditions and help you find an effective treatment plan.
What Is the Best Heart Healthy Diet for Heart Disease?
There are many diets that claim to improve your health, but not all of them are effective. Follow the best heart healthy diet so you can avoid heart disease.
Your diet plays a huge role in your overall health, especially when it comes to preventing and managing heart disease.
Common causes of heart disease, including high blood sugar and high cholesterol, are made worse by a poor diet. If you eat meals high in processed sugar, sodium, and fats, your heart will suffer for it. Therefore, the most heart-healthy diets are those that are high in fruits, vegetables, whole grains, and lean proteins.
Many different diets fit these criteria, such as the ever-popular DASH diet and the TLC diet. Perhaps the most effective is the Mediterranean diet, which supports not only heart health but also increases longevity and assists in weight control.
What Is the Mediterranean Diet?
As the name suggests, the Mediterranean diet is based on the types of food eaten by people living around the Mediterranean Sea. It became popular due to research that suggested people living in countries like Greece, France, and Italy experienced health benefits compared to those following the standard American diet.
In particular, researchers found that following a Mediterranean diet could drastically reduce your risk of developing heart disease, type two diabetes, Alzheimer’s disease, and cancer. People living in the Mediterranean region had fewer deaths caused by coronary heart disease and frequently lived longer, healthier lives.
In recent years, the Mediterranean diet has become a popular choice for anyone looking to slim down, but its primary focus is still on promoting healthy eating habits that help prevent heart disease.
Diet as a Heart Disease Treatment
Your regular diet plays a significant role in determining your risk factors for heart disease. If you consistently eat foods that are high in bad fats and cholesterol, which may also have large amounts of sugar and sodium, your heart health will suffer. On the other hand, if you make healthy choices for each meal, you can lower your likelihood of developing heart disease.
Of course, diet is far from the only possible heart disease treatment. You can combine a healthy Mediterranean diet with exercise to multiply its positive effects.
The Mediterranean Diet and Heart Disease
Following the Mediterranean diet can reduce your risk of developing the cardiovascular conditions that contribute to heart disease. Namely, it can lower your blood pressure by cutting out excessive sugar and salt, as well as help keep your cholesterol in check.
Unlike some other diets where you’re only meant to follow them for a few weeks at a time, you can safely follow the Mediterranean diet for years, making it a great option for long-term heart health.
How to Follow the Mediterranean Diet
There isn’t one well-defined set of rules or a strict meal plan associated with the Mediterranean diet. Instead, it focuses on eating a varied diet of primarily produce and whole grains alongside some healthy fats and the occasional glass of red wine.
What to Eat
Just about all whole fruits and vegetables are well suited to the Mediterranean diet, but you should opt for fruits with less sugar when you can. Try to have about seven to ten servings per day.
Rather than eating white bread, pasta, or pastries, choose whole grains, as these have a lower impact on your blood sugar levels.
While you should limit your consumption of saturated and trans fats, your body needs some fats to function. Focus on getting these fats from healthy sources, such as olive oil and fresh fish.
Aim to eat fish for at least two meals each week, as fish contains high levels of Omega-3 fatty acids that can reduce inflammation and lower your risk of having a stroke.
You can also have low-fat dairy options like Greek yogurt. Don’t forget about low-fat cheeses like feta and mozzarella too.
In addition to seafood and dairy, you can also get protein from plant-based sources like nuts and beans.
What to Limit or Avoid
While the Mediterranean diet lets you enjoy many different meals, there are some ingredients you should avoid. Avoid eating too many processed foods with lots of fats and sugars. Instead, stick to fresh, whole ingredients as often as you can.
Limit how often you have red meat as well, as it is higher in saturated fat than most plant or seafood sources of protein. Go for leaner cuts, and only have a steak or burger on rare occasions, if at all.
Keep your sodium levels in check by leaving salt out of most of your meals. Instead, you can use fresh spices and herbs to give your meals all of the flavor with none of the spikes in blood pressure.
Final Thoughts
Improving your health starts with altering your diet. Reducing your risk of heart disease is no exception to this rule.
The Mediterranean diet is very flexible, with plenty of options to suit any palette. Considering its positive effects on your heart and overall well-being, there’s no reason not to give it a try.
Advances in Treating Cholesterol to Manage Heart Disease
High cholesterol is one of the biggest contributors to heart disease. Luckily, there have been many advancements in how we monitor and reduce cholesterol.
Even though our bodies need cholesterol, too much of the ‘bad’ kind of cholesterol, called low-density lipoprotein (LDL), can cause serious health issues. These include plaque deposits that increase your risk of heart disease, heart attacks, or stroke.
Just as there have been many advancements in heart disease treatments, so too have there been advancements in how we treat high cholesterol as our knowledge of the condition improves. The more we learn about the relationship between high cholesterol and heart disease, the more effective modern heart disease treatment methods become.
Cholesterol and Heart Disease
As a significant contributor to heart disease, it’s important that cholesterol levels are kept under control. Otherwise, plaque continues to build up in the arteries, which raises your blood pressure and puts more strain on your heart. These plaque deposits can become blockages, making them especially dangerous.
That said, not all cholesterol is bad for you. Some can actually improve your health, despite our initial understanding of how it interacts with our bodies.
LDL and HDL
Previously, it was believed that all cholesterol was bad, and this is still a popular belief outside of the medical community. However, we now know that there are both good and bad types of cholesterol and that the good kind can be used to reduce the amount of bad cholesterol in our bodies.
LDL is considered bad cholesterol because it directly contributes to the arterial buildup of plaque. It comes from saturated and trans fats, which usually come from animal products and heavily processed foods, respectively.
High-density lipoproteins (HDLs) are considered good cholesterol. They’re responsible for bringing LDL to your liver, where it can then be broken down and discarded. Eating foods high in HDL like olive oil and certain fish can help you counteract the negative effects of a diet high in LDL.
Of course, even our knowledge of the distinction between LDL and HDL is continually evolving, allowing us to develop more effective treatment methods.
Advancements in Cholesterol and Heart Disease Treatment Methods
Modern methods for treating high cholesterol primarily involve the use of medications and changes to your diet and exercise habits.
Cholesterol Medications
Some medications are designed to reduce cholesterol production in your liver. These are known as ‘statins,’ and they include medications such as Simvastatin, Rosuvastatin, and the most common, Atorvastatin. While statins can reduce the overall level of cholesterol coming from your liver, they do not have any effect on dietary cholesterol, so they must be combined with healthy eating habits.
There are also many statin alternatives. These include fibrates, niacin or vitamin B3, and omega-3 supplements, which all lower triglycerides.
Reverse Cholesterol Transport
Not all methods used for treating high cholesterol and heart disease have to involve medications. You can significantly improve your heart health by using reverse cholesterol transport, which occurs when HDL transports cholesterol out of the arteries and back to the liver. This helps decrease the accumulation of LDLs in the arteries, meaning less opportunity for plaque formation.
While excessive amounts of LDL are known to clog arteries, just eliminating bad cholesterol from your diet isn’t enough. You also need to increase your HDL levels to combat the bad effects of overall high cholesterol efficiently. Studies show that people with higher than average HDL levels have the lowest risk of developing heart disease, especially if they’ve been including HDLs in their diet from a young age.
To take advantage of reverse cholesterol transport, you can use good nutrition in conjunction with the previously mentioned medications. Changing your diet is especially important, as it can prevent the development of heart disease altogether if you are committed to eating healthier. You can get HDLs from various foods, including beans, olive oil, fatty fish, fruit with high fiber content, nuts, and whole grains.
Final Thoughts
Moderating your cholesterol is a key part of keeping your heart healthy and reducing your risk of developing heart disease. The sooner you can improve your cholesterol, either through medications or lifestyle changes, the less risk you have of damaging your arteries and harming your heart, and the better your overall health will be.
How to Recognize the Symptoms of a Heart Attack
Heart attacks are serious and require you to react immediately.
Know the symptoms so you can identify a heart attack and seek the appropriate treatment.
Many people who suffer from heart disease don’t know they have it until they experience a heart attack.
Some heart attacks can seem to come out of nowhere, with almost no warning before they occur. However, most have warning signs that are much easier to detect when you know what you’re looking for.
Whether you believe you have heart disease or not, being able to spot the warning signs of a heart attack could save your life.
How to Recognize a Heart Attack
Knowing the warning signs is a key factor in getting medical help as soon as possible. If you brush off these symptoms as nothing to worry about, you could put yourself in greater danger, so always treat any possible symptoms seriously.
Chest Pain
By far, the most common symptom of a heart attack is chest pain. This usually feels like discomfort accompanied by a squeezing feeling of pressure on the left side or center of your chest. Pain may be severe or fairly mild, so don’t ignore it just because the pressure or tightness is light.
Chest pain is a fairly general symptom, and it can have many causes completely unrelated to a heart attack or heart disease. Chest pain that comes on suddenly with no clear cause is often an indicator of a potential heart attack, and it’s best not to take any risks. This kind of pain is even more likely to be caused by a heart attack if it is accompanied by other common symptoms.
Upper Body Pain
In addition to chest pain, a heart attack can cause pain that radiates through other areas of your upper body. Left arm pain is common, especially for men, but you can also experience pain or tightness in your upper back, neck, and jaw.
Shortness of Breath
Heart palpitations and chest tightness can leave you feeling out of breath during a heart attack. You may struggle to take full, deep breaths, even if you were previously sitting or laying down without issues. If you experience shortness of breath without a clear cause, it could be that you are having a heart attack or another medical emergency.
Nausea
Heart attacks can leave you feeling nauseated, which can sometimes lead to vomiting. Nausea and vomiting are common to many different health conditions both major and mild, but when associated with chest pain and shortness of breath, it might be another indicator of a heart attack.
Heart Attack Differences Between Men and Women
Men and women often experience different symptoms for heart attacks.
Men are more likely to feel chest pain, especially pain that feels like squeezing. Shortness of breath, nausea, and pain in the jaw, back, or neck are all common symptoms for men too. Men often experience severe pain in their left arms during a heart attack as well.
For women, left arm pain is much rarer, and the range of symptoms is usually wider. In addition to the regular symptoms, women may also experience sudden and serious fatigue, fainting, or indigestion. Women may not even have chest pain during a heart attack, so it’s especially important to stay vigilant for these less common symptoms.
How to React If You Are Having a Heart Attack
If you think you might be having a heart attack, you should seek medical treatment as quickly as possible. Delaying treatment even by a few minutes can put your life in jeopardy.
First, don’t try to drive yourself to the hospital. It’s better to call 911, as the EMTs who arrive in the ambulance can provide emergency care on the way to the hospital. Additionally, if you lose control while driving, you could get in an accident, delaying help even further and potentially injuring yourself and others.
While waiting for the ambulance, follow any directions the dispatcher gives you. If you’re at home, unlock the door and sit or lie down nearby so the EMTs can reach you faster.
After Receiving Medical Care
Once you see a doctor and you’re on the road to recovery, always follow their advice to improve your heart health and prevent future heart attacks. If you continue the same bad habits as before, you’ll likely make your heart disease worse.
About one in five people who have a heart attack will have another within five years, and this risk only goes up if you don’t take care of your body.
If you follow your doctor’s advice and take any necessary prescriptions, you can greatly lower your chances of experiencing a second heart attack and improve your overall health.
Final Thoughts
Heart attacks can be unexpected and frightening, but acting quickly increases your chances of making a full recovery. Make sure you understand the signs of a heart attack and always ask for assistance from friends or bystanders right away.
5 Types of Medications Used to Combat Heart Disease
Your doctor can prescribe various types of medications to counteract the harmful effects of heart disease. Here are five of the most commonly prescribed types.
If you’ve been diagnosed with heart disease, you’re not alone. Nearly half of all American adults are affected by cardiovascular disease. So, it’s important to make every effort to improve your heart health and minimize your risk of developing dangerous complications.
Lifestyle changes that keep your cholesterol and blood pressure in check can help, but for some people, this won’t be enough. In these cases, your doctor may want to prescribe medications to treat your heart disease.
Even though these medications have the same general goal, their level of effectiveness can be different for different people. Learn about the various types of medications that are frequently prescribed so you and your doctor can work together to decide on the best treatment.
Medications Used for Heart Disease Treatment
There are dozens of different heart disease medications, and many of them help reduce the damage heart disease causes in different ways. Some focus on improving blood flow, while others target factors like cholesterol and plaque buildup.
Metoprolol
Metoprolol is a type of medication known as a beta blocker. This means it lowers your blood pressure by reducing the speed and force of your heartbeats. They can also help widen your veins and arteries, which may have become narrowed, thus facilitating improved circulation.
Metoprolol is also used to reduce the overall risk of heart failure. People with heart disease who take metoprolol have a higher survival rate from a heart attack.
Common side effects include dizziness, fatigue, stomach pain, and nausea.
Statins
Statins are a type of drug that can reduce the amount of cholesterol produced by your liver. This helps regulate your cholesterol levels, which in turn, lowers your risk of developing heart disease or further damaging your heart.
Too much bad cholesterol can create plaque deposits in your arteries, limiting blood flow throughout your body. By reducing the amount of harmful cholesterol, you can minimize your risk of having a heart attack or stroke caused by heart disease and blocked arteries.
Commonly prescribed statins include Atorvastatin, Lovastatin, Rosuvastatin, Pravastatin, and Simvastatin.
Blood Thinners
Blood thinners are also called anticoagulants because they prevent coagulation, or clotting, in your blood. Clots can cause arterial blockages that make heart attacks or strokes more likely, so they’re frequently prescribed to people with heart disease.
Note that blood thinners can be dangerous if you exceed your prescribed dosage. If you sustain an injury such as a cut or laceration, your blood won’t be able to clot and stop the bleeding like usual. This means that applying pressure to the area and seeking medical attention for continued bleeding will be necessary.
Practice extra caution and be careful to avoid combining blood thinners with any medication that can interact negatively with them. Always read labels to know what medications to avoid with blood thinners.
Plavix
Plavix, also known as Clopidogrel, is a type of blood thinner that can reduce your risk of having a stroke or heart attack.
You may experience side effects such as increased bleeding, bruising, and itching.
Diltiazem
Diltiazem functions as a type of antihypertensive drug known as a calcium channel blocker.
Calcium channel blockers lower your blood pressure by inhibiting the movement of calcium into your heart and artery cells. Diltiazem is commonly used in the treatment of the arrhythmia atrial fibrillation.
Talk to Your Doctor About Heart Disease
For each of the medications above, you’ll need a prescription from your doctor. This means you will need to schedule follow-up appointments at least once a year to renew your prescription and perform any necessary tests to monitor your heart disease.
Always follow all instructions when taking any medication. Read the label and keep an eye out for any side effects that could potentially be dangerous. Talk to your doctor if you feel lightheaded, frequently nauseous, or extremely fatigued, and always get physician approval before you stop taking any heart disease medication.
Final Thoughts
Medications do their part to prevent or treat heart disease, but you can’t rely on medication alone.
Instead, you will have to make lifestyle changes like eating right, maintaining ideal body weight, and getting enough exercise each day to support your heart health.
If you use these methods alongside any necessary medications, you’ll greatly increase their effectiveness.
What Can You Do to Avoid Developing Heart Disease?
Heart disease can lead to serious complications like heart attacks and strokes. Learn how you can improve your coronary health and avoid heart disease.
Heart disease can have serious consequences for your overall health. It increases your risk of having a stroke or heart attack, which can be life-threatening.
Luckily, avoiding heart disease doesn’t necessarily need to involve surgical procedures or complex medication regimens.
You can protect your heart health by simply making adjustments to your lifestyle.
Lifestyle Changes for Reducing Your Risk of Heart Disease
Heart disease can be the product of genetics, but it’s often the result of the daily choices you make.
Should you buy fast food after work, or should you go home and ma dke yourself a healthy meal with vegetables and whole grains? Should you go on that run you planned, or should you watch another episode of your favorite TV show?
These decisions become habits, good or bad, and their effect adds up over time.
If you want to reduce your risk of heart disease, you can start by exercising more frequently, reducing stress, quitting smoking, and eating healthier.
Get Active
Just a few minutes of exercise each day has a significant impact on your cardiovascular health. People who are physically fit have a much lower risk of developing heart disease, especially when routine exercise is combined with other methods of staying healthy.
You don’t have to be a professional athlete to strengthen your heart. Start by doing a few jumping jacks or push-ups each day, and then work in a short jog around the block. Make sure to include exercise that increases your heart rate for the best cardiovascular benefits.
If you’re struggling to stick to your workout routine, try making it more fun with unconventional exercises. Rather than hitting the gym, try dancing or playing an active sport like soccer or tennis with some friends. Any kind of movement that can raise your heart rate or strengthen your muscles makes a big difference.
Practice Stress Reduction
Sustained stress in your daily life isn’t just bad for your mood. It’s also bad for your heart since stress can raise your blood pressure.
If your stress comes from a hectic lifestyle, you might not be able to drop all your responsibilities. However, you can still take time out of your day to destress and improve your health.
Schedule a time every day to just relax and do something fun. Take your work outside for a nice change in your environment. Try out meditation or mindfulness exercises.
Any of these practices can help you feel a little more zen and keep your stress levels under control.
Stop Smoking
Smoking can cause all sorts of health problems, including heart disease. Heavy smoking increases your risk of developing a clot in your arteries, which inhibits blood flow and can lead to a heart attack or stroke.
It can be hard to quit cold turkey, even if you know the toll smoking is taking on your health. If you’re a heavy smoker, you might find it more helpful to slowly decrease how much you smoke each day until quitting seems more achievable.
You can try nicotine patches to help reduce cravings and withdrawal symptoms.
Avoid situations that function as triggers for smoking. Smoking may also be a way for you to alleviate stress or other unpleasant feelings, so replace it with other methods for dealing with these feelings like fun hobbies and breathing exercises.
Diet Control as Heart Disease Treatment
What you eat is a hugely influential factor in your overall health. If you eat a lot of high-fat, high-sugar, and high-cholesterol foods, you are actively contributing to your risk of heart disease.
Work to eliminate these foods from your diet and replace them with healthier options like plant-based proteins and whole, fresh foods. You can follow a heart healthy diet like the Mediterranean diet if you prefer a more guided approach to nutrition.
Final Thoughts
Managing your risk of heart disease can be as simple as changing what you eat, how often you work out, and how you deal with stress. These are small changes, but they can add up to a powerful impact on your well-being, especially if you make changes in many different areas of your life.
If you’ve fallen into bad health habits, it can be tough to change your approach. Start with one small change, like smoking one less cigarette or making sure at least one of your meals each day is homemade. These small changes will have a cumulative effect over time, even if they feel very easy to make in the moment.
Swap out bad habits for healthy ones to do everything you can to live a life free of heart disease.